'Challenges in Diagnosis: Ovarian Dysgerminoma Presenting as Torsion in a Prepubertal Girl: A Case Report' - an article in the 'Advocacy for Maternal and Women’s Health' collection by Jaypee Brothers Publishing on #ScienceOpen:
🔗 https://www.scienceopen.com/document?vid=bb11c9a0-bda7-4c45-89ae-6b6591884eb7
Challenges in Diagnosis: Ovarian Dysgerminoma Presenting as Torsion in a Prepubertal Girl: A Case Report
<div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d5873679e139"> <!-- named anchor --> </a> <h5 class="section-title" id="d5873679e140">Aim and background</h5> <p dir="auto" id="d5873679e142">Dysgerminoma is the most common malignant germ cell tumor of the ovary; it usually affects people under the age of twenty and usually manifests as abdominal pain, distention, and a palpable mass. Just 10% of ovarian tumors in patients under the age of 18 are malignant, with functional cysts accounting for the majority of cases. </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d5873679e144"> <!-- named anchor --> </a> <h5 class="section-title" id="d5873679e145">Case description</h5> <p dir="auto" id="d5873679e147">Here, we describe an uncommon case of an 11-year-old girl who had abdominal discomfort, and torsion and was diagnosed with dysgerminoma. Following a right-sided salpingo-oophorectomy to preserve fertility, the patient was diagnosed with stage III dysgerminoma on histopathology due to omental metastasis. The patient underwent adjuvant chemotherapy due to tumor metastasis to the omentum. </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d5873679e149"> <!-- named anchor --> </a> <h5 class="section-title" id="d5873679e150">Conclusion</h5> <p dir="auto" id="d5873679e152">Ideally, young patients receiving adjuvant treatment for metastases should have fertility-sparing surgery. Postoperative monitoring and regular follow-up are essential for the early detection and management of patients with metastases, even without any disease indications. </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d5873679e154"> <!-- named anchor --> </a> <h5 class="section-title" id="d5873679e155">Clinical significance</h5> <p dir="auto" id="d5873679e157">This case underscores the importance of considering dysgerminoma in pediatric patients who present with abdominal symptoms, and highlights the importance of management strategies for treating this rare ovarian malignancy in young individuals. </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d5873679e159"> <!-- named anchor --> </a> <h5 class="section-title" id="d5873679e160">How to cite this article</h5> <p dir="auto" id="d5873679e162">Gupta S, Motwani V, Kalwaniya DS, <i>et al</i>. Challenges in Diagnosis: Ovarian Dysgerminoma Presenting as Torsion in a Prepubertal Girl: A Case Report. J South Asian Feder Obst Gynae 2024;16(5):564–567. </p> </div>
Lessons learned from the pandemic: expanding the collaboration between clinical and logistics activities in a hospital
<div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d7331674e285"> <!-- named anchor --> </a> <h5 class="section-title" id="d7331674e286">Purpose</h5> <p dir="auto" id="d7331674e288">The Covid-19 pandemic generated significant changes in the operating methods of hospital logistics departments. The objective of this research is to understand how these changes took place, what collaboration mechanisms were developed with clinical authorities and, to what extent, logistics and clinical care activities should be decoupled to maximize each area's contribution? </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d7331674e290"> <!-- named anchor --> </a> <h5 class="section-title" id="d7331674e291">Design/methodology/approach</h5> <p dir="auto" id="d7331674e293">The case study is selected to investigate practices implemented during the COVID-19 pandemic in hospitals in Canada. The pandemic presented an opportunity to contrast practices implemented in response to this crisis with those historically used in this environment. </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d7331674e295"> <!-- named anchor --> </a> <h5 class="section-title" id="d7331674e296">Findings</h5> <p dir="auto" id="d7331674e298">The strategy of decoupling logistical tasks of an operational nature from clinical activities is well-founded and helps free clinical staff from tasks for which they are not trained. However, the decoupling of operational tasks should be combined with an integration of the clinical information flow to the logistics hub players. With this clinical information, the logistics hub can generate its full potential enabling better inventory management decisions to be made. </p> </div><div xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" class="section"> <a class="named-anchor" id="d7331674e300"> <!-- named anchor --> </a> <h5 class="section-title" id="d7331674e301">Originality/value</h5> <p dir="auto" id="d7331674e303">The concept of decoupling is studied to identify configurations that offer the best benefits for clinical staff. </p> </div>
A rare case of <i>Trichosporon inkin</i> bloodstream infection in an immunocompetent patient: Diagnostic challenges and antigenic cross-reactivity
<p xmlns:xsi="http://www.w3.org/2001/XMLSchema-instance" dir="auto" id="d6664000e99"> <i>Trichosporon inkin</i> is a rare opportunistic pathogen typically associated with superficial infections but can also cause invasive infections, particularly in immunocompromised hosts. Here, we report a rare case of <i>T. inkin</i> bloodstream infection in an immunocompetent male with a history of cerebral hemorrhage surgery. The patient presented with fever, limb twitching, and brain lesions. Blood cultures revealed fungal growth, which was initially misidentified as <i>Trichosporon ovoides</i> by mass spectrometry but was later confirmed as <i>T. inkin</i> through ITS and IGS1 sequencing. The isolate exhibited low MICs for azoles and amphotericin B but high MICs for echinocandins. Notably, the patient’s serum tested positive for cryptococcal antigen and <i>Aspergillus</i> galactomannan, despite the absence of clinical signs of cryptococcosis or aspergillosis. The <i>T. inkin</i> isolate expresses cryptococcal antigen but not galactomannan cross-reactive antigens when cultured in standard media. However, it expresses galactomannan cross-reactive antigens when cultured in human whole blood. This case highlights diagnostic challenges, including antigenic cross-reactivity and misidentification, and emphasizes the role of host-pathogen interactions in antigen expression. Our findings underscore the need for improved diagnostics and cautious interpretation of fungal antigen tests. This report expands the understanding of <i>T. inkin</i> infections and provides insights into their clinical management. </p>
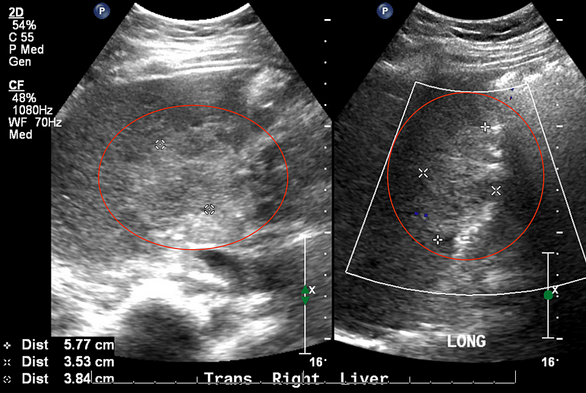
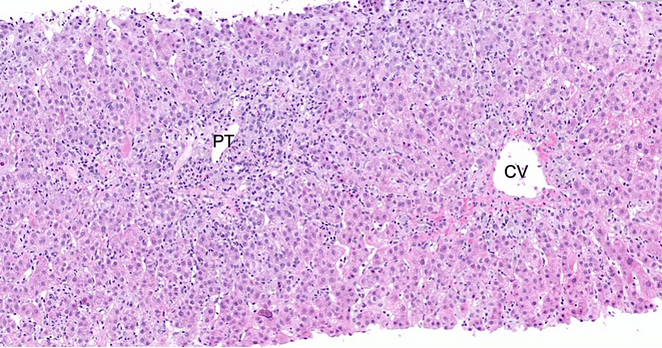
約有14~53%的確診者有肝臟功能障礙並發症,而在此案例報告中分享了一確診後沒感染肝炎病毒且抗核抗體、抗平滑肌抗體等並未上升,最後診斷為自身抗體陰性自體免疫肝炎的案例
並建議沒有看到相關抗體上升時仍需注意自體免疫肝炎的可能性❗️
Seronegative Autoimmune Hepatitis: A Rare Manifestation of COVID-19
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus responsible for the coronavirus pandemic in 2019, commonly causes hepatic dysfunction. Liver injury ranges from mildly elevated liver enzymes to fulminant liver failure. Interestingly, there are cases that suggest a relationship between autoimmune hepatitis (AIH) in patients who either contracted coronavirus disease in 2019 (COVID-19) or were vaccinated against severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). We present a case of a 39-year-old female without a significant past medical history who presented with two weeks of jaundice, abdominal pain, nausea, and diarrhea. She had significantly elevated liver enzymes and conjugated hyperbilirubinemia. She also tested positive for SARS-CoV-2 but denied any respiratory symptoms; her vaccination status was up to date. She denied taking hepatotoxic agents, and the workup was negative for acute viral hepatitis. The F-actin antibody level was 22 units, but serum immunoglobulin (IgG), anti-nuclear (ANA), anti-smooth muscle, anti-mitochondrial, anti-liver/kidney microsomal-1, anti-soluble liver antigen, and anti-neutrophil cytoplasmic antibodies levels were not elevated. Computerized tomography of the abdomen and pelvis revealed hepatic hemangiomas. Eventually, a liver biopsy was performed, and histology showed active lymphoplasmacytic hepatitis with prominent regenerative changes and areas of confluent necrosis. The histologic findings, along with the patient's clinical course, were suggestive of autoimmune hepatitis. The patient was started on systemic steroids with an improvement of abdominal pain and jaundice, as well as an improvement of her liver chemical profile. She was discharged with plans for hepatology clinic follow-up. Here, we present a rare case of seronegative AIH in a patient with a recent COVID-19 infection and discuss the potential underlying mechanism. We call for further investigation into the relationship between autoimmune dysfunction and COVID-19, as well as the pathophysiology behind it. Analyzing how the virus causes autoimmune dysfunction may allow clinicians to more effectively treat patients suffering from sequelae of COVID-19 infection, and it is important not to exclude autoimmune hepatitis from the differential based on the initial autoimmune workup.