Rethinking human resources for malaria control and elimination in Africa
The comprehensive policy review by Halima Mwenesi and colleagues “Rethinking human resources and capacity building needs for malaria control and elimination in Africa” argues that the stagnation in global malaria progress is fundamentally a human resources crisis rather than solely a biological or technical failure.
The authors posit that the current workforce is insufficient in number and ill-equipped with the necessary skills to navigate the complex transition from malaria control to elimination.
It is a critical indictment of the status quo in malaria training and offers a roadmap for structural reform.
This article summarizes key points from the policy review and examines how The Geneva Learning Foundation’s peer learning-to-action model could be used by national programmes to transform the health workforce.
The mismatch between training and operational needs
The authors identify a severe imbalance in training priorities where capacity building has historically favored biomedical and basic sciences such as entomology and parasitology.
While essential, this focus has led to a neglect of operational, translational, and implementation sciences.
The report highlights that while the global community produces high-level scientists who understand the parasite, it fails to produce “translational scientists” who can bridge the gap between global guidelines and local realities.
This has resulted, they argue, in a workforce lacking the practical competencies to operationalize complex elimination strategies that require precision and adaptation.
The deficit in leadership and social sciences
A major finding is the specific deficit in so-called “soft skills” and social sciences which are increasingly critical as programs move toward elimination.
The authors argue that modern malaria control requires competencies in leadership, health diplomacy, anthropology, sociology, and political analysis.
Program managers currently lack the training to navigate complex political landscapes, mobilize domestic resources, or engage effectively with communities to sustain interventions.
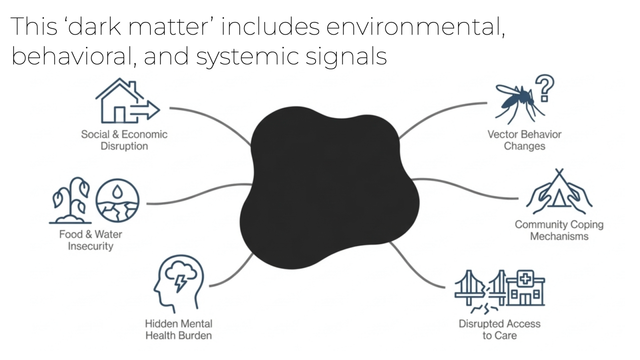
The review emphasizes that understanding community behavior and social determinants is as critical as understanding vector behavior but this is rarely reflected in curricula.
Data illiteracy and the failure of surveillance
The paper identifies pervasive “data illiteracy” across the workforce.
Health workers collect vast amounts of data to satisfy donor reporting requirements but often lack the skills to interpret or use it for local decision-making.
This results in a “data-rich but information-poor” environment.
As countries move toward elimination, the need for real-time, granular surveillance becomes paramount.
The current workforce is unable to perform the rapid data analysis required to detect and respond to outbreaks at the sub-national level.
Fragmentation and lack of coordination
The review critiques the fragmentation of investments in training, capacity-building, and technical assistance driven by donor agendas.
It notes a lack of coordination among donors and agencies which leads to a proliferation of uncoordinated short courses and workshops that do not necessarily align with national strategic plans.
This fragmentation is exacerbated by a lack of data on the workforce itself.
Many countries lack a central registry of malaria personnel which makes it impossible to forecast needs, plan for attrition, or manage career pathways.
The call for structural transformation
The authors call for a radical shift toward “South-South” collaboration where African institutions take the lead in training.
They advocate for moving away from ad hoc workshops toward institutionalized, long-term capacity building.
Crucially, they recommend the use of digital platforms to democratize access to knowledge for mid-level and community-based cadres who are often excluded from elite fellowships.
How can learning science help transform malaria training investments into tangible health worker performance?
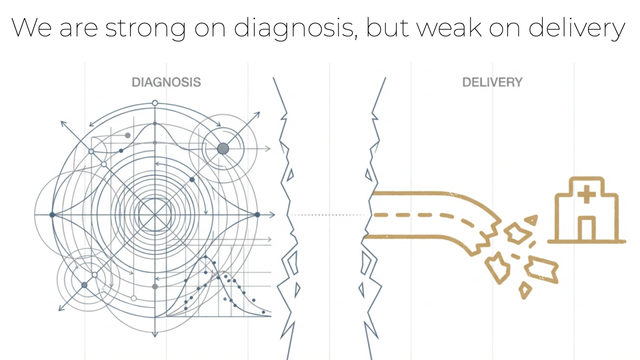
For a global health epidemiologist accustomed to viewing disease control through the lens of biological interventions and coverage rates, the human resource crisis described by Mwenesi and colleagues represents a “delivery failure” of validated tools.
The Geneva Learning Foundation (TGLF) learning science model functions as a structural intervention designed to repair broken delivery mechanisms in global health and humanitarian response.
The following analysis translates the TGLF approach into terms recognizable to an epidemiologist or program manager who operates with the assumption that training is primarily about the transmission of technical knowledge.
Moving from passive transmission to implementation fidelity
Epidemiologists understand that a vaccine with high efficacy in a trial often has low effectiveness in the real world due to poor administration or cold chain failure.
Similarly, Mwenesi et al. identify that technical malaria guidelines fail because the “human infrastructure” cannot implement them.
Traditional training assumes that if you lecture health workers on a protocol, which is a transmission of information, they will execute it.
This is a “single-loop” assumption.
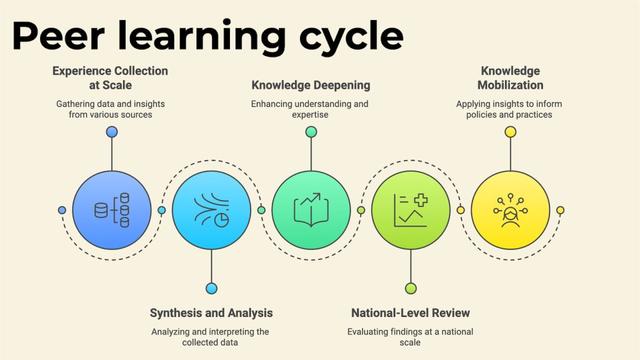
The TGLF model introduces an “implementation loop.”
Instead of merely receiving information, learners in the TGLF network must design a micro-project to apply the new guideline in their specific district, execute it, and report back on the results using their own local data.
This turns the workforce from passive recipients of protocols into active testers of implementation fidelity.
It directly addresses the “translational science” gap identified in the paper by forcing the learner to translate theory into practice immediately.
Sceptics often argue that this approach places an undue burden on an already overworked workforce.
However, the TGLF model embeds learning into the workflow itself.
This is not additional work but rather “learning-based work.”
Participants do not create hypothetical projects.
They identify a bottleneck they are currently facing, such as a specific pocket of malaria transmission, and use the learning cycle to address it.
This transforms the training from an external interruption into an operational support mechanism.
By embedding learning into the workflow, it operationalizes Mwenesi’s call for translational science.
It considers the daily struggle of the health worker as a form of structured scientific inquiry: they hypothesize a solution, test it, and report the results.
This is implementation as science.
Operationalizing data use for local decision-making
Mwenesi notes that health workers collect data but do not use it.
In the TGLF model, data is not something sent “up” to the ministry.
It is the raw material for peer support and feedback.
In a TGLF peer learning exercise, a district medical officer in Ghana shares their case management data to compare performance with a peer in Uganda.
They share because they want to, not because they are required to.
This creates a social incentive to understand and analyze one’s own data.
It builds the “data literacy” the authors call for not through abstract statistics courses but through the practical necessity of explaining one’s own performance to a colleague.
This process transforms data from a compliance burden into a tool for local problem-solving.
Is there a risk that peer learning will pool ignorance?
Is there a valid concern regarding the risk of “pooled ignorance” where peers might reinforce incorrect practices?
The TGLF model mitigates this through “structured emergence.”
The model does not dismiss expert knowledge but uses global guidelines as the “anchor” for local problem-solving.
In this system, a health worker cannot simply state an opinion.
They must submit an action plan that is peer-reviewed against a rubric derived from WHO guidelines.
This process ensures fidelity to technical standards while allowing for necessary local adaptation.
The aggregation of thousands of these peer-reviewed plans creates a new form of rigorous, practice-based evidence that complements expert guidance.
Scaling “soft skills” through structured peer review
The review calls for leadership and diplomacy skills but notes these are hard to teach in workshops.
The TGLF model builds these skills implicitly through its pedagogical structure.
When a participant submits an action plan, they must receive and respond to critical feedback from peers in other countries.
They must negotiate differing viewpoints and defend their technical choices.
This mimics the “health diplomacy” and leadership dynamics required in real-world program management.
Furthermore, because they must engage community stakeholders to implement their projects, they practice the anthropological and social engagement skills Mwenesi identifies as missing.
They learn leadership not by studying a theory of leadership but by leading a change initiative in their facility.
While some experts argue that soft skills require “hard contact” in physical spaces, TGLF results suggest that physical proximity often limits a worker to their known environment and existing biases.
The TGLF model introduces a form of “cosmopolitan localism.”
When a nurse in rural Nigeria must explain her challenge to a peer in urban India, she is forced to articulate her context with a clarity and diplomacy not required when speaking to a neighbor.
This defiance of distance fosters a quantum leap in communication capabilities.
Participants report that the skills learned in negotiating these digital, cross-cultural peer relationships directly translate to better engagement with their physical-world colleagues and community leaders.
Addressing the incentive structure and correcting expertise asymmetry
The paper critiques the “brain drain” and the reliance on experts from the Global North.
TGLF operationalizes the “South-South” collaboration recommended by the authors by creating a flat digital hierarchy.
In this model, the “expert” is not a visiting consultant from Geneva but a peer who has successfully solved the problem in their own context.
A nurse in Nigeria learns how to improve bed net usage from a nurse in Kenya who solved that exact refusal issue last month.
This actually results in greater interest, comprehension, and use of official guidelines.
It also validates local knowledge and creates the “critical mass of thinking professionals” that Mwenesi argues is essential for elimination.
It shifts the source of authority from external experts to the collective intelligence of the network.
Transforming the economy of per diem
A common critique of moving away from face-to-face training is the reliance of health workers on per diems for financial survival.
Mwenesi implies that the current system is unsustainable.
The TGLF model operates on the evidence that per diem-driven training often restricts access to a “training aristocracy” of recurrent participants while excluding the frontline workers who most need the knowledge.
TGLF replaces the financial incentive with a professional survival incentive.
In the Nigeria Immunization Collaborative, over 4,300 health workers participated without per diems.
They did so because the program addressed the specific pain points of their daily work.
This filters the workforce for “positive deviants,” or those with high intrinsic motivation who are most likely to drive elimination efforts, rather than those primarily motivated by daily subsistence allowances.
A “surveillance system” for human resources and performance
Finally, the review notes the lack of registries and data on the workforce itself.
The TGLF digital network acts as a real-time sensor of workforce capacity.
By engaging thousands of health workers simultaneously, the platform generates data on who is active, what problems they are facing, and where their skills are deficient.
For an epidemiologist, this is equivalent to a surveillance system for human resources.
It provides the visibility needed to forecast gaps and target interventions precisely, replacing the “blind” proliferation of uncoordinated workshops with a data-driven approach to capacity building.
Regarding concerns that digital platforms fail in low-resource settings due to poor connectivity, TGLF utilizes a “cognitively quiet” design that functions on low-bandwidth connections and mobile devices.
This design respects the technological reality of the African context.
Data from the Teach to Reach program, which has engaged over 60,000 participants in remote, ongoing peer learning activities , demonstrates that when the technology is adapted to the user rather than the other way around, participation rates exceed those of physical workshops.
This scale allows for the identification of systemic patterns and workforce gaps that would be invisible in a smaller, face-to-face cohort.
Reference
Mwenesi, H., Mbogo, C., Casamitjana, N., Castro, M.C., Itoe, M.A., Okonofua, F., Tanner, M., 2022. Rethinking human resources and capacity building needs for malaria control and elimination in Africa. PLOS Glob Public Health 2, e0000210. https://doi.org/10.1371/journal.pgph.0000210
Reda Sadki (2023). How do we reframe health performance management within complex adaptive systems?. Reda Sadki: Learning to make a difference. https://doi.org/10.59350/mx5qr-qet97
Reda Sadki (2024). Prioritizing the health and care workforce shortage: protect, invest, together. Reda Sadki: Learning to make a difference. https://doi.org/10.59350/zzqr4-9g482
Reda Sadki (2024). Protect, invest, together: strengthening health workforce through new learning models. Reda Sadki: Learning to make a difference. https://doi.org/10.59350/g24b4-7fj64
Reda Sadki (2024). What is double-loop learning in global health?. Reda Sadki: Learning to make a difference. https://doi.org/10.59350/s4xtw-b7274
Reda Sadki (2024). World Malaria Day 2024: We need new ways to support health workers leading change with local communities. Reda Sadki: Learning to make a difference. https://doi.org/10.59350/yrn1r-hpz62
#brainDrain #cosmopolitanLocalism #dataQualityAndUse #doubleLoopLearning #HalimaMwenesi #healthWorkerMotivation #healthWorkerPerformance #healthWorkforce #HRH #implementationScience #leadership #learningStrategy #learningBasedWork #localization #malaria #peerLearning #performance #softSkills #TeachToReach #translationalScience