HPV and Cervical Cancer: The importance of Early Detection
Cervical cancer is one of the most preventable cancers affecting women today, yet it remains a significant global health threat, especially in low- and middle-income countries. The primary cause? A common virus: HPV (Human Papillomavirus).
The good news? With vaccination, routine screening, and early treatment, most cases of cervical cancer can be prevented or treated before they become life-threatening.
What Is HPV?
HPV is the most common sexually transmitted infection (STI) in the world.Most sexually active people will contract it at some point, often without even knowing it. There are over 100 types of HPV, but only about 14 are considered high-risk for causing cancer.
Two high-risk types, HPV 16 and 18, are responsible for approximately 70% of cervical cancer cases worldwide.
HPV spreads through skin-to-skin contact, usually during vaginal, anal, or oral sex. In many cases, the immune system clears the infection within 1 to 2 years. However, when high-risk types persist, they can cause abnormal changes in cervical cells, which may eventually lead to cancer.
HPV and Other Types of Cancer
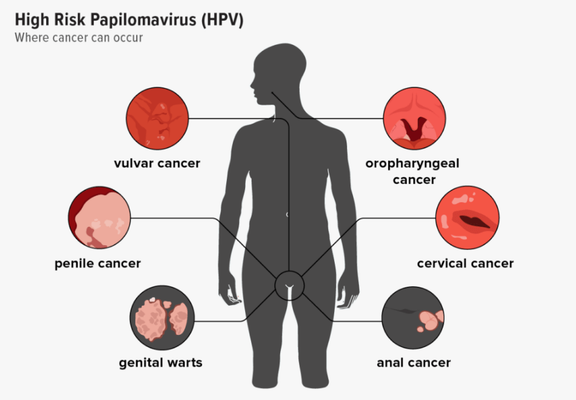
While cervical cancer is the most well-known HPV-related cancer, the virus can also cause:
- Anal cancer
- Vaginal and vulvar cancer
- Penile cancer
- Oropharyngeal cancer (throat, base of the tongue, and tonsils)
These are primarily associated with HPV 16, one of the high-risk strains.
The HPV vaccine helps protect against the strains that cause most of these cancers. This is why it is recommended for both boys and girls starting from age 9, and in some countries, for adults up to age 45, ideally before becoming sexually active.
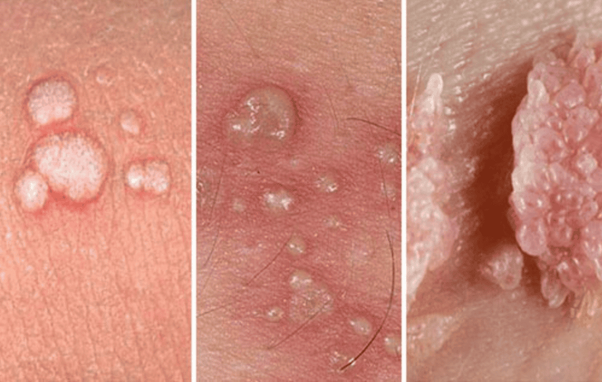
What About Genital Warts?
Not all HPV types cause cancer. Some low-risk strains, such as HPV 6 and 11, can lead to genital warts which are small, soft growths on or around the genitals. While these are not dangerous, they can be emotionally distressing and uncomfortable.
Fortunately, the same HPV vaccine also protects against these low-risk strains.
What Is the Cervix, and Why Is It Vulnerable?
The cervix is the lower, narrow part of the uterus that connects to the vagina. It is essentially the gateway between the womb and the outside world. It plays a critical role in:
- Menstruation – allowing blood to exit the uterus
- Reproduction – producing mucus that can aid or block sperm
- Childbirth – expanding to allow delivery of a baby
Due to its exposure and structure, the cervix is particularly susceptible to HPV infection, which can gradually cause cellular damage and precancerous changes.
What Is Cervical Cancer?
Cervical cancer occurs when abnormal cells in the cervix grow uncontrollably. The development is usually slow, often taking years, which allows time for early detection and intervention.
How Cervical Cancer Progresses: The Stages
Doctors group cervical cancer into stages to describe how far it has spread:
- Stage 0 – Precancer. Abnormal cells are only on the cervix’s surface.
- Stage I – Cancer is limited to the cervix.
- Stage II – Spread to nearby tissues (e.g., upper vagina)
- Stage III – Reaches the pelvic wall or blocks urinary paths.
- Stage IV – Spread to distant organs like the liver, bladder, or lungs.
Early detection can stop this progression before it becomes life-threatening.
Why Early Detection Matters
Cervical cancer often develops without noticeable symptoms, which is why routine screening is crucial. Common screening tools include:
- Pap smears – detects abnormal changes in cervical cells.
- HPV testing – identifies high-risk strains of the virus.
- Colposcopy – a close visual examination of the cervix.
These tests can detect issues before cancer develops or catch it at its most treatable stage.
How Are HPV and Cervical Cancer Connected?
Here Let’s break it down:
1. A person is exposed to a high-risk HPV type.
2. The virus infects the cervical cells.
3. If the virus persists, it causes abnormal cell changes.
4. Without detection or treatment, these changes can progress to cancer.
Nearly all cases of cervical cancer are caused by persistent HPV infections.
Prevention: What You Can Do
1. Get the HPV Vaccine
- Safe and effective
- Best between ages 9 and 12 (before sexual activity)
- Approved in many countries up to age 45
- Protects against the types responsible for most cervical cancers and genital warts
If you weren’t vaccinated as a child, talk to your doctor about catch-up doses.
2. Schedule Regular Pap Smears and HPV Tests
- Pap smears starting at age 21
- HPV testing often begins at age 30
- Self-sampling kits are becoming available in some regions
Ask your healthcare provider what schedule is best based on your age, health, and country’s guidelines.
3. Practice Safer Sex
While condoms don’t fully prevent HPV, they greatly reduce the risk. Additional precautions include:
- Limiting the number of sexual partners
- Open communication with partners about sexual health
- Regular testing and health checkups
Signs and Symptoms of Cervical Cancer
Early-stage cervical cancer typically causes no symptoms. As it progresses, warning signs may include:
- Abnormal vaginal bleeding (after sex, between periods, or after menopause)
- Pelvic or lower back pain
- Unusual vaginal discharge
- Pain during sexual intercourse
If you experience any of these symptoms, see a healthcare provider immediately.
The Bottom Line
Cervical cancer is preventable. With the right tools such as vaccination, screening, education, and early treatment, we can protect ourselves and others.
Take Action Today:
✅ Get vaccinated
✅ Book your screening
✅ Talk to friends and family
✅ Share this post. It could save a life.
References
- World Health Organization (WHO): HPV and Cervical Cancer
- CDC: HPV Vaccine Information
- American Cancer Society: What Is Cervical Cancer?
- NHS: Cervical Screening