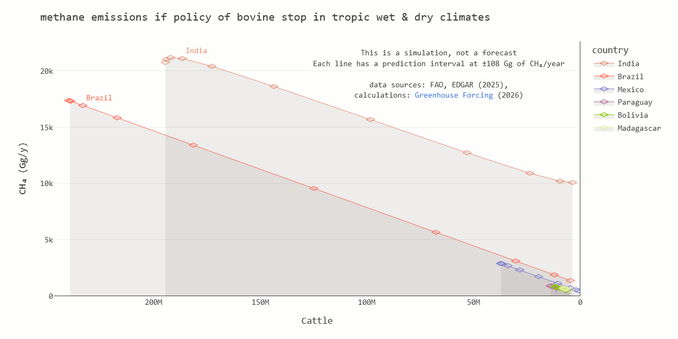
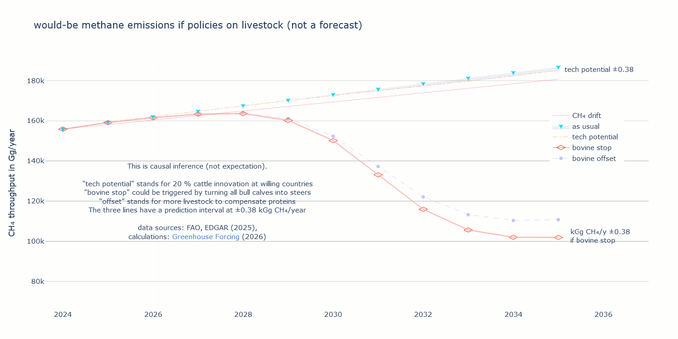
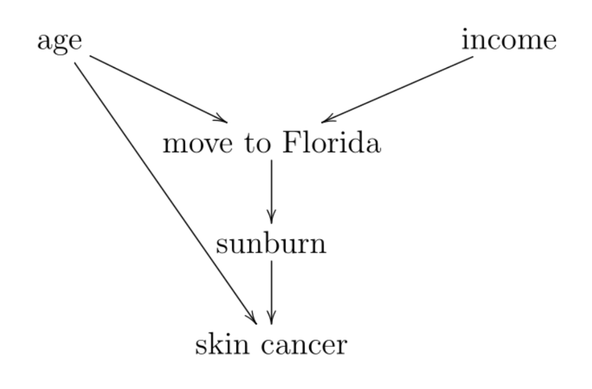
New study uses causal analysis to demonstrate big reductions in carbon emissions if fewer bovines.
In ten years, methane emissions from all activities if bovine stop would be 80 % of methane emissions from all activities if no intervention.
Results and causation are presented at https://doi.org/10.5281/zenodo.19019693
#carbon #causality #causalInference #causation #confounding #counterFactuals #emissions #GHG #methane #offPolicy #policy #publicPolicy