Myocardial infarction: self amplifying RNA for heart protective hormone delivered by intramuscular injection of lipid nanoparticles. Encouraging results in animal trials. https://www.science.org/doi/abs/10.1126/science.adu9394?af=R
The Mayo Clinic and Anumana have developed 3 ECG-AI models that together pinpoint hearts at risk for potentially devastating attacks some 3 years earlier. #AI #ECG #coronaryarterydisease #myocardial #echo #mayo #anumana
https://www.instagram.com/p/CzUOXNWR0i9/
Results of this study show that #cardiac CT can quantify #myocardial extracellular volume (ECV) and yield results comparable to cardiac MR in cardiac amyloidosis patients. (Hidetaka Hayashi et al.)
🔗 https://link.springer.com/article/10.1007/s00330-023-10129-w
Myocardial extracellular volume quantification in cardiac amyloidosis: a comparative study between cardiac computed tomography and magnetic resonance imaging - European Radiology
Objectives Myocardial extracellular volume (ECV) on computed tomography (CT), an alternative to cardiac magnetic resonance (CMR), has significant practical clinical advantages. However, the consistency between ECVs quantified via CT and CMR in cardiac amyloidosis (CA) has not been investigated sufficiently. Therefore, the current study investigated the application of CT-ECV in CA with CMR-ECV as the reference standard. Methods We retrospectively evaluated 31 patients with CA who underwent cardiac CT and CMR. Pearson correlation analysis was performed to investigate correlations between CT-ECV and CMR-ECV at each segment. Further, correlations between ECV and clinical parameters were assessed. Results There were no significant differences in the mean global ECVs between CT scan and CMR (51.3% ± 10.2% vs 50.0% ± 10.5%). CT-ECV was correlated with CMR-ECV at the septal (r = 0.88), lateral (r = 0.80), inferior (r = 0.79), anterior (r = 0.77) segments, and global (r = 0.87). In both CT and CMR, the ECV had a weak to strong correlation with high-sensitivity cardiac troponin T level, a moderate correlation with global longitudinal strain, and an inverse correlation with left ventricular ejection fraction. Further, the septal ECV and global ECV had a slightly higher correlation with the clinical parameters. Conclusions Cardiac CT can quantify myocardial ECV and yield results comparable to CMR in patients with CA. Moreover, a significant correlation between CT-ECV and clinical parameters was observed. Thus, CT-ECV can be an imaging biomarker and alternative to CMR-ECV. Clinical relevance statement Cardiac CT can quantify myocardial ECV and yield results comparable to CMR in patients with CA, and CT-ECV can be used clinically as an imaging biomarker and alternative to CMR-ECV. Key Points • A significant correlation was found between CT myocardial extracellular volume and cardiac MR myocardial extracellular volume in patients with cardiac amyloidosis. • In CT and cardiac MR, the myocardial extracellular volume correlated well with high-sensitivity cardiac troponin T level, global longitudinal strain, and left ventricular ejection fraction. • CT myocardial extracellular volume can be an imaging biomarker and alternative to cardiac MR myocardial extracellular volume.
Recovery of #cardiac function in patients with ST-segment elevation #myocardial #infarction found to be better in reverse left ventricular remodeling (r-LVR) group than in the group without r-LVR over time. (Jianing Cui et al.)
🔗 https://link.springer.com/article/10.1007/s00330-023-09907-3
Cardiac magnetic resonance for the early prediction of reverse left ventricular remodeling in patients with ST-segment elevation myocardial infarction - European Radiology
Objectives To evaluate the changes in cardiac magnetic resonance (CMR) characteristics and investigate the predictors of reverse left ventricular remodeling (r-LVR) in ST-segment elevation myocardial infarction (STEMI) patients. Materials and methods Eighty-six STEMI patients (median 56 years) were retrospectively studied. The patients were divided into r-LVR and without r-LVR groups. CMR analysis included LV volume, infarct characteristics, and global and regional myocardial function. The strain and displacement were assessed by CMR-feature tracking. The predictors of r-LVR were analyzed by the logistic regression method. Results There were 37 patients in the r-LVR group and 49 patients in the without r-LVR group. At initial CMR, there was no difference in LV volume and global cardiac function between the two groups. However, the infarct zone radial and longitudinal displacements were higher in the r-LVR group (p < 0.05, respectively). At the second CMR, the r-LVR group showed higher LVEF, lower LV volume, and total enhanced mass (all p < 0.05). The infarct zone radial and circumferential strains and radial displacement were higher in the r-LVR group (all p < 0.05). The r-LVR group had better recovery of myocardial injury and function. Of note, microvascular obstruction (MVO) mass (odds ratio: 0.779 (0.613–0.989), p = 0.041) and infarct zone peak longitudinal displacement (PLD) (odds ratio: 1.448 (1.044–2.008), p = 0.026) were independent predictors of r-LVR. Conclusions At initial CMR, there were no differences in global cardiac function between the two groups, but infarct zone displacements were higher in the r-LVR group. The r-LVR group had better recovery of cardiac function. In addition, MVO mass and infarct zone PLD were independent predictors of r-LVR. Clinical relevance statement Our study assessed changes in cardiac structure, function, and tissue characteristics after STEMI by CMR, investigated the best predictors of r-LVR in STEMI patients, and laid the foundation for the development of new parameter-guided treatment strategies for STEMI patients. Key Points • At initial CMR, the reverse left ventricular remodeling (r-LVR) group had less myocardial damage and higher infarct zone displacement, but there were no differences in global function between the two groups. • Both groups showed recovery of myocardial injury and cardiac function over time, but the r-LVR group had less enhanced mass and better cardiac function compared to the without r-LVR group at the second CMR. • Microvascular obstruction mass and infarct zone peak longitudinal displacement by cardiac magnetic resonance feature-tracking were significant predictors of r-LVR in STEMI patients.
Head-to-head comparison of #cardiac MR techniques pits parametric techniques against convential cardiac MR to visually differentiate #ischemic from non-ischemic #myocardial injury patterns. (Charlotte Jahnke et al.)
🔗 https://link.springer.com/article/10.1007/s00330-023-09905-5
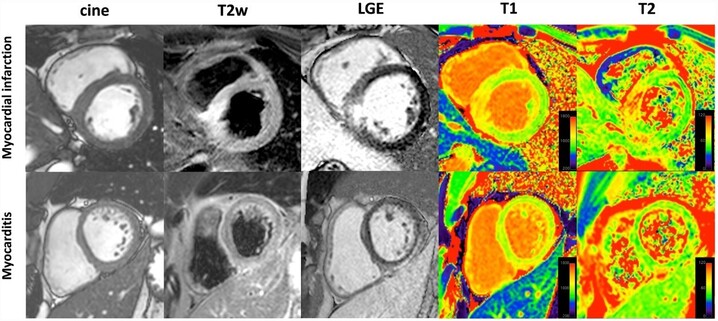
Differentiation of acute non-ST elevation myocardial infarction and acute infarct-like myocarditis by visual pattern analysis: a head-to-head comparison of different cardiac MR techniques - European Radiology
Objectives Parametric cardiac magnetic resonance (CMR) techniques have improved the diagnosis of pathologies. However, the primary tool for differentiating non-ST elevation myocardial infarction (NSTEMI) from myocarditis is still a visual assessment of conventional signal-intensity-based images. This study aimed at analyzing the ability of parametric compared to conventional techniques to visually differentiate ischemic from non-ischemic myocardial injury patterns. Methods Twenty NSTEMI patients, twenty infarct-like myocarditis patients, and twenty controls were examined using cine, T2-weighted CMR (T2w) and late gadolinium enhancement (LGE) imaging and T1/T2 mapping on a 1.5 T scanner. CMR images were presented in random order to two experienced fully blinded observers, who had to assign them to three categories by a visual analysis: NSTEMI, myocarditis, or healthy. Results The conventional approach (cine, T2w and LGE combined) had the best diagnostic accuracy with 92% (95%CI: 81–97) for NSTEMI and 86% (95%CI: 71–94) for myocarditis. The diagnostic accuracies using T1 maps were 88% (95%CI: 74–95) and 80% (95%CI: 62–91), 84% (95%CI: 67–93) and 74% (95%CI: 54–87) for LGE, and 83% (95%CI: 66–92) and 73% (95%CI: 53–87) for T2w. The accuracies for cine (72% (95%CI: 52–86) and 60% (95%CI: 38–78)) and T2 maps (62% (95%CI: 40–79) and 47% (95%CI: 28–68)) were significantly lower compared to the conventional approach (p < 0.001 and p < 0.0001). Conclusions The conventional approach provided a reliable visual discrimination between NSTEMI, myocarditis, and controls. The diagnostic accuracy of a visual pattern analysis of T1 maps was not significantly inferior, whereas the diagnostic accuracy of T2 maps was not sufficient in this context. Clinical relevance statement The ability of parametric compared to conventional CMR techniques to visually differentiate ischemic from non-ischemic myocardial injury patterns can avoid potentially unnecessary invasive coronary angiography and help to shorten CMR protocols and to reduce the need of gadolinium contrast agents. Key Points • A visual differentiation of ischemic from non-ischemic patterns of myocardial injury is reliably achieved by a combination of conventional CMR techniques (cine, T2-weighted and LGE imaging). • There is no significant difference in accuracies between visual pattern analysis on native T1 maps without providing quantitative values and a conventional combined approach for differentiating non-ST elevation myocardial infarction, infarct-like myocarditis, and controls. • T2 maps do not provide a sufficient diagnostic accuracy for visual pattern analysis for differentiating non-ST elevation myocardial infarction, infarct-like myocarditis, and controls.
#Myocardial salvage index (MSI) shows potential in predicting major adverse #cardiovascular events (MACE) in ST-segment elevation myocardial #infarction (STEMI) patients. (Zhengguang Xiao et al.)
💻 👉 https://link.springer.com/article/10.1007/s00330-023-09739-1
The prognostic value of myocardial salvage index by cardiac magnetic resonance in ST-segment elevation myocardial infarction patients: a systematic review and meta-analysis - European Radiology
Objective To assess the prognostic value of myocardial salvage index (MSI) by cardiac magnetic resonance (CMR) in ST-segment elevation myocardial infarction (STEMI) patients. Methods We systematically searched PubMed, Embase, Web of Science, Cochrane Central, China National Knowledge Infrastructure, and Wanfang Data to identify primary studies reporting MSI in STEMI patients with major adverse cardiovascular events (MACE) comprised of death, myocardial reinfarction, and congestive heart failure. The MSI and MACE rates were pooled. The bias of risk was assessed using the Quality In Prognosis Studies tool. The evidence level was rated based on the meta-analysis of hazard ratio (HR) and 95% confidence interval (CI) of MSI for predicting MACE. Results Eighteen studies were included covering twelve unique cohorts. Eleven cohorts measured MSI using T2-weighted imaging and T1-weighted late gadolinium enhancement, while one cohort applied T2-mapping and T1-mapping. The pooled MSI (95% CI) was 44% (39 to 49%; 11 studies, 2946 patients), and the pooled MACE rate (95% CI) was 10% (7 to 14%; 12 studies, 311/3011 events/patients). Seven prognostic studies overall showed low risk of bias. The HR (95% CI) per 1% increase of MSI for MACE was 0.95 (0.92 to 0.98; 5 studies, 150/885 events/patients), and HR (95% CI) of MSI < median versus MSI > median for MACE was 5.62 (3.74 to 8.43; 6 studies, 166/1570 events/patients), both rated as weak evidence. Conclusions MSI presents potential in predicting MACE in STEMI patients. The prognostic value of MSI using advanced CMR techniques for adverse cardiovascular events needs further investigation. Clinical relevance statement Seven studies supported the MSI to serve as a predictor for MACE in STEMI patients, indicating its potential as a risk stratification tool to help manage expectations for these patients in clinical practice. Key Points • The pooled infarct size (95% CI) and area at risk (95% CI) were 21% (18 to 23%; 11 studies, 2783 patients) and 38% (34 to 43%; 10 studies, 2022 patients), respectively. • The pooled rates (95% CI) of cardiac mortality, myocardial reinfarction, and congestive heart failure were 2% (1 to 3%; 11 studies, 86/2907 events/patients), 4% (3 to 6%; 12 studies, 127/3011 events/patients), and 3% (1 to 5%; 12 studies, 94/3011 events/patients), respectively. • The HRs (95% CI) per 1% increase of MSI for cardiac mortality and congestive heart failure were 0.93 (0.91 to 0.96; 1 study, 14/202 events/patients) and 0.96 (0.93 to 0.99; 1 study, 11/104 events/patients), respectively, but the prognostic value of MSI for myocardial re-infraction has not been measured.
Why Does COVID-19 Cause Severe Illness in Some Patients but Not Others?
Factors linked to disease outcomes included viral load, frequencies of certain cell types such as #cytotoxic #natural #killer (#NK) cells, various #inflammatory #states, and markers of #myocardial #damage.
In participants who died of the infection, #viral #loads persisted and even started to rise over time. By contrast, viral loads steadily declined in those with milder infections.
The activation of cell types such as cytotoxic NK cells increased in the milder cases as participants’ immune systems ramped up in response to the infection, while these cells decreased in the more severe groups.
Furthermore, participants who were sickest had higher levels of inflammatory markers upon hospitalization that increased over time, while patients in the milder groups showed an opposite pattern
< Yale School of Medicine
#Medical #sflorg
https://www.sflorg.com/2023/06/med06122302.html
Fully quantitative #myocardial perfusion reserve (MPR) could provide excellent diagnostic performance for detecting hemodynamically significant #coronary #artery disease (CAD). (Shi-hai Zhao et al.)
🔗 https://link.springer.com/article/10.1007/s00330-023-09689-8
Fully automated pixel-wise quantitative CMR-myocardial perfusion with CMR-coronary angiography to detect hemodynamically significant coronary artery disease - European Radiology
Objectives We applied a fully automated pixel-wise post-processing framework to evaluate fully quantitative cardiovascular magnetic resonance myocardial perfusion imaging (CMR-MPI). In addition, we aimed to evaluate the additive value of coronary magnetic resonance angiography (CMRA) to the diagnostic performance of fully automated pixel-wise quantitative CMR-MPI for detecting hemodynamically significant coronary artery disease (CAD). Methods A total of 109 patients with suspected CAD were prospectively enrolled and underwent stress and rest CMR-MPI, CMRA, invasive coronary angiography (ICA), and fractional flow reserve (FFR). CMRA was acquired between stress and rest CMR-MPI acquisition, without any additional contrast agent. Finally, CMR-MPI quantification was analyzed by a fully automated pixel-wise post-processing framework. Results Of the 109 patients, 42 patients had hemodynamically significant CAD (FFR ≤ 0.80 or luminal stenosis ≥ 90% on ICA) and 67 patients had hemodynamically non-significant CAD (FFR ˃ 0.80 or luminal stenosis < 30% on ICA) were enrolled. On the per-territory analysis, patients with hemodynamically significant CAD had higher myocardial blood flow (MBF) at rest, lower MBF under stress, and lower myocardial perfusion reserve (MPR) than patients with hemodynamically non-significant CAD (p < 0.001). The area under the receiver operating characteristic curve of MPR (0.93) was significantly larger than those of stress and rest MBF, visual assessment of CMR-MPI, and CMRA (p < 0.05), but similar to that of the integration of CMR-MPI with CMRA (0.90). Conclusions Fully automated pixel-wise quantitative CMR-MPI can accurately detect hemodynamically significant CAD, but the integration of CMRA obtained between stress and rest CMR-MPI acquisition did not provide significantly additive value. Key Points • Full quantification of stress and rest cardiovascular magnetic resonance myocardial perfusion imaging can be postprocessed fully automatically, generating pixel-wise myocardial blood flow (MBF) and myocardial perfusion reserve (MPR) maps. • Fully quantitative MPR provided higher diagnostic performance for detecting hemodynamically significant coronary artery disease, compared with stress and rest MBF, qualitative assessment, and coronary magnetic resonance angiography (CMRA). • The integration of CMRA and MPR did not significantly improve the diagnostic performance of MPR alone.
A short news story I wrote reporting on a study that found the shape of your #heart can help predict risk for atrial fibrillation.
The first few paragraphs (most of the story):
Rounder hearts predict future heart failure, a-fib
Greater left ventricular sphericity showed 47% greater incidence of #cardiomyopathy
MAY 2023 -- Not everyone’s heart is quite the same shape and its shape changes over time – but this could help predict who’s at risk for #cardiomyopathy.
A study in CellPress, where researchers analysed cardiac MRIs of over 30,000 people, found that variations in left ventricle sphericity in normal hearts predicted risk for cardiomyopathy and related outcomes.
Researchers hypothesized that beyond size and function, the shape of hearts might carry extra details about heart health. To study this, they used data from a large biobank with cardiac imaging data to help analyze variation in cardiac morphology in normal populations.
They noted “Cardiomyopathies of different etiologies often result in a similar end-stage phenotype of a more round, spherical ventricle. Among individuals with known cardiac disease, increased sphericity of the left ventricle (LV) has been associated with adverse outcomes, including ventricular arrhythmias and death.”
It also stated that “within the spectrum of normal LV chamber size and systolic function, there exists variation in LV sphericity, and this variation may be a marker of cardiac risk with genetic underpinnings.”
The researchers turned to artificial intelligence to help analyze 38,897 cardiac MRIs from the U.K. Biobank database. The cohort had undergone cardiac MRIs and had normal LV end-diastolic volume, normal LV end-systolic volume, and normal LV ejection fraction.
The team looked at LV sphericity and whether it predicted incident cardiomyopathy as well as clinical manifestations such as atrial fibrillation, heart failure, and #cardiac arrest. Other factors were taken into account such as body mass index, pulse rate, #hypertension, diabetes, and prior #myocardial infarction.
“We found that individuals with spherical hearts were 31% more likely to develop atrial fibrillation and 24% more likely to develop cardiomyopathy,” said Dr. David Ouyang in a press release. He is coauthor of the study and a cardiologist at Cedars Sinai in California....
The full story is online. Sorry, its password protected. It's accessible, free to #doctors and #pharmacists #myocardial #medicine #MedicalPost #MedMastodon #cardiology @medmastodon
MY NEWS REPORT: https://www.canadianhealthcarenetwork.ca/rounder-hearts-predict-future-heart-failure-fib
THE STUDY: https://www.cell.com/action/showPdf?pii=S2666-6340%2823%2900069-7