Myocardial infarction: self amplifying RNA for heart protective hormone delivered by intramuscular injection of lipid nanoparticles. Encouraging results in animal trials. https://www.science.org/doi/abs/10.1126/science.adu9394?af=R
Engineering a broken heart ❤️🩹
In this #preprint, highlighted by Theodora Stougiannou, the authors develop a method to study Myocardial Infarct healing in vitro.
Read the preLight! ⬇️ 👀
Heart Scar-In-A-Dish: Tissue Culture Platform to Study Myocardial Infarct Healing In Vitro - preLights
In this preprint, the authors employ a cryoinjury model to produce a three-dimensional (3D) Myocardial Infarction (MI)-Engineered Heart Tissue (EHT) platform that spatially/temporally mimics the evolution of MI.
Crazy 😬
Plastics, Fossil Carbon, and the Heart ❤️(and #Brain 🧠 )
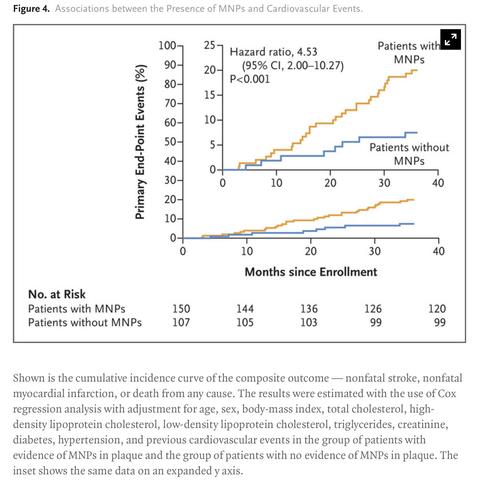
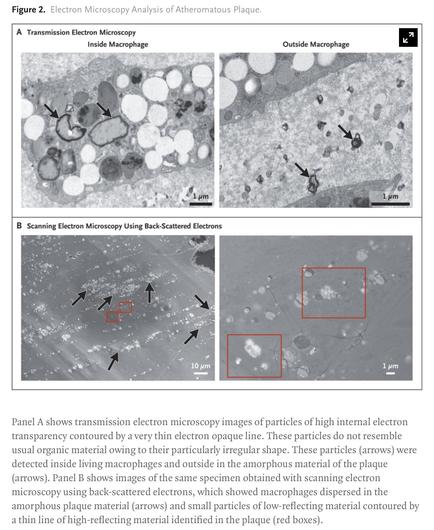
Microplastics and nanoplastics were detectable in the excised plaque of 58% of the patients 😨
The presence of #microplastics or #nanoplastics in #carotid #artery plaque was associated with a subsequent risk of nonfatal myocardial #infarction, nonfatal #stroke, or #death from any cause that was 2.1 times that in patients whose plaques did not contain microplastics or nanoplastics.
Patients with microplastics or nanoplastics in their plaque tissue also had elevated expression of circulating inflammatory markers
#heart #heartdisease
https://www.nejm.org/doi/full/10.1056/NEJMe2400683
Recovery of #cardiac function in patients with ST-segment elevation #myocardial #infarction found to be better in reverse left ventricular remodeling (r-LVR) group than in the group without r-LVR over time. (Jianing Cui et al.)
🔗 https://link.springer.com/article/10.1007/s00330-023-09907-3
Cardiac magnetic resonance for the early prediction of reverse left ventricular remodeling in patients with ST-segment elevation myocardial infarction - European Radiology
Objectives To evaluate the changes in cardiac magnetic resonance (CMR) characteristics and investigate the predictors of reverse left ventricular remodeling (r-LVR) in ST-segment elevation myocardial infarction (STEMI) patients. Materials and methods Eighty-six STEMI patients (median 56 years) were retrospectively studied. The patients were divided into r-LVR and without r-LVR groups. CMR analysis included LV volume, infarct characteristics, and global and regional myocardial function. The strain and displacement were assessed by CMR-feature tracking. The predictors of r-LVR were analyzed by the logistic regression method. Results There were 37 patients in the r-LVR group and 49 patients in the without r-LVR group. At initial CMR, there was no difference in LV volume and global cardiac function between the two groups. However, the infarct zone radial and longitudinal displacements were higher in the r-LVR group (p < 0.05, respectively). At the second CMR, the r-LVR group showed higher LVEF, lower LV volume, and total enhanced mass (all p < 0.05). The infarct zone radial and circumferential strains and radial displacement were higher in the r-LVR group (all p < 0.05). The r-LVR group had better recovery of myocardial injury and function. Of note, microvascular obstruction (MVO) mass (odds ratio: 0.779 (0.613–0.989), p = 0.041) and infarct zone peak longitudinal displacement (PLD) (odds ratio: 1.448 (1.044–2.008), p = 0.026) were independent predictors of r-LVR. Conclusions At initial CMR, there were no differences in global cardiac function between the two groups, but infarct zone displacements were higher in the r-LVR group. The r-LVR group had better recovery of cardiac function. In addition, MVO mass and infarct zone PLD were independent predictors of r-LVR. Clinical relevance statement Our study assessed changes in cardiac structure, function, and tissue characteristics after STEMI by CMR, investigated the best predictors of r-LVR in STEMI patients, and laid the foundation for the development of new parameter-guided treatment strategies for STEMI patients. Key Points • At initial CMR, the reverse left ventricular remodeling (r-LVR) group had less myocardial damage and higher infarct zone displacement, but there were no differences in global function between the two groups. • Both groups showed recovery of myocardial injury and cardiac function over time, but the r-LVR group had less enhanced mass and better cardiac function compared to the without r-LVR group at the second CMR. • Microvascular obstruction mass and infarct zone peak longitudinal displacement by cardiac magnetic resonance feature-tracking were significant predictors of r-LVR in STEMI patients.
#Myocardial salvage index (MSI) shows potential in predicting major adverse #cardiovascular events (MACE) in ST-segment elevation myocardial #infarction (STEMI) patients. (Zhengguang Xiao et al.)
💻 👉 https://link.springer.com/article/10.1007/s00330-023-09739-1
The prognostic value of myocardial salvage index by cardiac magnetic resonance in ST-segment elevation myocardial infarction patients: a systematic review and meta-analysis - European Radiology
Objective To assess the prognostic value of myocardial salvage index (MSI) by cardiac magnetic resonance (CMR) in ST-segment elevation myocardial infarction (STEMI) patients. Methods We systematically searched PubMed, Embase, Web of Science, Cochrane Central, China National Knowledge Infrastructure, and Wanfang Data to identify primary studies reporting MSI in STEMI patients with major adverse cardiovascular events (MACE) comprised of death, myocardial reinfarction, and congestive heart failure. The MSI and MACE rates were pooled. The bias of risk was assessed using the Quality In Prognosis Studies tool. The evidence level was rated based on the meta-analysis of hazard ratio (HR) and 95% confidence interval (CI) of MSI for predicting MACE. Results Eighteen studies were included covering twelve unique cohorts. Eleven cohorts measured MSI using T2-weighted imaging and T1-weighted late gadolinium enhancement, while one cohort applied T2-mapping and T1-mapping. The pooled MSI (95% CI) was 44% (39 to 49%; 11 studies, 2946 patients), and the pooled MACE rate (95% CI) was 10% (7 to 14%; 12 studies, 311/3011 events/patients). Seven prognostic studies overall showed low risk of bias. The HR (95% CI) per 1% increase of MSI for MACE was 0.95 (0.92 to 0.98; 5 studies, 150/885 events/patients), and HR (95% CI) of MSI < median versus MSI > median for MACE was 5.62 (3.74 to 8.43; 6 studies, 166/1570 events/patients), both rated as weak evidence. Conclusions MSI presents potential in predicting MACE in STEMI patients. The prognostic value of MSI using advanced CMR techniques for adverse cardiovascular events needs further investigation. Clinical relevance statement Seven studies supported the MSI to serve as a predictor for MACE in STEMI patients, indicating its potential as a risk stratification tool to help manage expectations for these patients in clinical practice. Key Points • The pooled infarct size (95% CI) and area at risk (95% CI) were 21% (18 to 23%; 11 studies, 2783 patients) and 38% (34 to 43%; 10 studies, 2022 patients), respectively. • The pooled rates (95% CI) of cardiac mortality, myocardial reinfarction, and congestive heart failure were 2% (1 to 3%; 11 studies, 86/2907 events/patients), 4% (3 to 6%; 12 studies, 127/3011 events/patients), and 3% (1 to 5%; 12 studies, 94/3011 events/patients), respectively. • The HRs (95% CI) per 1% increase of MSI for cardiac mortality and congestive heart failure were 0.93 (0.91 to 0.96; 1 study, 14/202 events/patients) and 0.96 (0.93 to 0.99; 1 study, 11/104 events/patients), respectively, but the prognostic value of MSI for myocardial re-infraction has not been measured.
#Medical #sflorg
https://www.sflorg.com/2023/06/med06122302.html
Inflammation associated with invasive pneumococcal disease the unifying mechanism? #sepsis #infection #MI #myocardial #infarction #medicine #IDMastodon
Risk of acute myocardial infarction among patients with laboratory-confirmed invasive pneumococcal disease: a self-controlled case series study | Clinical Infectious Diseases | Oxford Academic
https://academic.oup.com/cid/advance-article-abstract/doi/10.1093/cid/ciad065/7030946
risk of acute myocardial infarction among patients with laboratory-confirmed invasive pneumococcal disease: a self-controlled case series study
We identified an elevated incidence of hospitalizations with acute myocardial infarction (AMI) during periods associated with laboratory-confirmed invasive pneu
Analytica Chimica Acta Volume 1239, 25 January 2023, 340673
https://doi.org/10.1016/j.aca.2022.340673
#ramaneffect #sers #infarction