How long can adverse physical symptoms last after #COVID19 infection? 🦠
⚡ In this joint 1st-authorship w/Shen, Joyce & Didriksen, we investigate this in 65000 adults across 4 nations up to 27 months (>2 years)
🧵
As many in the #global population have contracted C19, persistence of different symptoms after #SARSCoV2 infection has become a key #publichealth concern
Symptoms continuing over 2 months after infection has been identified as #LongCOVID or post-C19 condition
https://www.medrxiv.org/content/10.1101/2023.04.18.23288720v1
COVID-19 illness severity and 2-year prevalence of physical symptoms: an observational study in Iceland, Sweden, Norway and Denmark
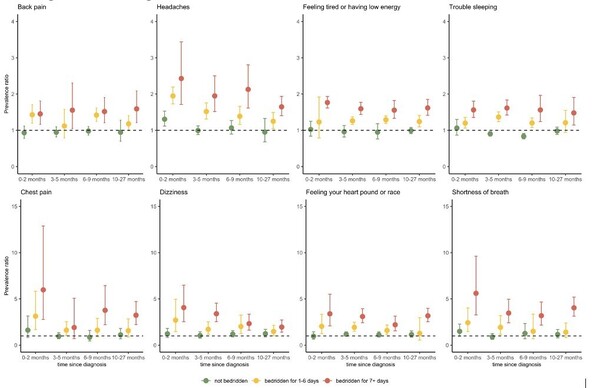
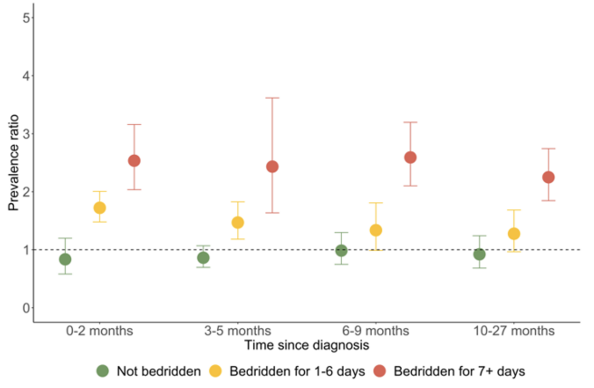
Background Persistence of physical symptoms after SARS-CoV-2 infection is a major public health concern, although evidence from large observational studies remain scarce. We aimed to assess the prevalence of physical symptoms in relation to acute illness severity up to more than 2-years after diagnosis of COVID-19. Methods This multinational study included 64 880 adult participants from Iceland, Sweden, Denmark, and Norway with self-reported data on COVID-19 and physical symptoms from April 2020 to August 2022. We compared the prevalence of 15 physical symptoms, measured by the Patient Health Questionnaire (PHQ-15), among individuals with or without a confirmed COVID-19 diagnosis, by acute illness severity, and by time since diagnosis. We additionally assessed the change in symptoms in a subset of Swedish adults with repeated measures, before and after COVID-19 diagnosis. Findings During up to 27 months of follow-up, 22 382 participants (34.5%) were diagnosed with COVID-19. Individuals who were diagnosed with COVID-19, compared to those not diagnosed, had an overall 37% higher prevalence of severe physical symptom burden (PHQ-15 score ≥ 15, adjusted prevalence ratio [PR] 1.37 [95% confidence interval [CI] 1.23-1.52]). The prevalence was associated with acute COVID-19 severity: individuals bedridden for seven days or longer presented with the highest prevalence (PR 2.25[1.85-2.74]), while individuals never bedridden presented with similar prevalence as individuals not diagnosed with COVID-19 (PR 0.92 [0.68-1.24]). The prevalence was statistically significantly elevated among individuals diagnosed with COVID-19 for eight of the fifteen measured symptoms: shortness of breath, chest pain, dizziness, heart racing, headaches, low energy/fatigue, trouble sleeping, and back pain. The analysis of repeated measurements rendered similar results as the main analysis. Interpretation These data suggest an elevated prevalence of some, but not all, physical symptoms during up to more than 2 years after diagnosis of COVID-19, particularly among individuals suffering a severe acute illness. Funding This work was mainly supported by grants from NordForsk (COVIDMENT, grant number 105668 and 138929) and Horizon2020 (CoMorMent, 847776). See Acknowledgements for further details on funding. Evidence before the study As the majority of the global population has contracted COVID-19, persistence of physical symptoms after SARS-CoV-2 infection ( Long COVID or post COVID-19 condition) has become a major public health concern. We searched PubMed for studies assessing physical symptoms after COVID-19, published by March 22, 2023. The search term was (physical symptoms after covid) AND LitCLONGCOVID [Pubmed filter]. We reviewed 82 studies, after excluding those not on humans or not published in English. High prevalence of multiple physical symptoms, mainly fatigue, shortness of breath, headache, muscle and chest pain, has been reported, mostly based on small samples of hospitalized patients confined to three to six months after diagnosis. A comprehensive assessment of long-term prevalence of physical symptoms beyond six months after diagnosis and among non-hospitalized patients is lacking. Added value of this study We included 64 880 participants from the general population of four Nordic countries, of whom 22 382 had been diagnosed with COVID-19 up to 2 years earlier (<1% hospitalized due to COVID-19). Individuals diagnosed with COVID-19 reported a 37% higher prevalence of overall severe physical symptom burden compared to individuals not diagnosed with COVID-19. We found that shortness of breath, chest pain, dizziness, headaches, and low energy/fatigue were particularly increased among individuals with COVID-19 diagnosis. Individuals bedridden for seven days or more during the acute illness phase (9.6% of the patients) showed the greatest and most persistent elevation in prevalence of severe physical symptoms while individuals not bedridden during the acute COVID-19 illness showed no increase in prevalence of physical symptoms compared to those not diagnosed. Implications of the available evidence Our findings provide timely and valuable evidence to demonstrate the constitution of Long COVID and the long-term health consequences after recovery from COVID-19 in the general population. The long-term risk of severe physical symptom burden is distinctly associated with acute illness severity, highlighting the importance of sustained monitoring of physical symptoms among the group of patients who suffered severe acute illness course. ### Competing Interest Statement O.A.A. is a consultant to cortechs.ai and has received speaker's honorarium from Lundbeck, Sunovion and Janssen. All other authors declare no conflict of interest. ### Funding Statement This work was supported by grants from NordForsk through the funding to Mental morbidity trajectories in COVID-19 across risk populations of five nations (COVIDMENT, grant number 105668), and from NordForsk through the funding to Long-term health sequels of COVID-19 infections and mitigation responses in Nordic populations (grant number 138929); the EU Horizon 2020 Research and Innovation Action Grant (CoMorMent, grant no. 847776). HA was supported by the Research Council of Norway (RCN 324 620). QS was supported by the Outstanding Clinical Discipline Project of Shanghai Pudong (Grant No.: PWYgy2021-02) and the Fundamental Research Funds for the Central Universities. Data collection in DBDS was funded by the Independent Research Fund Denmark (0214-00127B). KL was supported by the Estonian Research Council through grant number PSG615 and funding of the Estonian subproject of NordForsk project number 105668. UAV has received grants for the current work from Nordforsk and Horizon2020 as well as grants outside the current work from the Icelandic Research Fund, Swedish Research Council, Swedish Cancer Society and the European Research Council. ### Author Declarations I confirm all relevant ethical guidelines have been followed, and any necessary IRB and/or ethics committee approvals have been obtained. Yes The details of the IRB/oversight body that provided approval or exemption for the research described are given below: National Bioethics Committee as well as the National Data Protection Authority of Iceland University gave ethical approval for this work with regard to data from Icelandic cohort (NBC no. 20-073, 21-071); Ethics committee of Karolinska Institutet gave ethical approval for this work with regard to data from Swedish cohort (no. 2020-01785); Regional Committee for Medical Research Ethics of University of Oslo gave ethical approval for this work with regard to data from Norwegian cohort (reference number: 125510); Zealand and Central Denmark Regional Committees on Health Research Ethics (SJ-740 and M-2009237) and the Data Protection Agency (P-2019-99) of Region Zealand gave ethical approval for this work with regard to data from Danish cohort. I confirm that all necessary patient/participant consent has been obtained and the appropriate institutional forms have been archived, and that any patient/participant/sample identifiers included were not known to anyone (e.g., hospital staff, patients or participants themselves) outside the research group so cannot be used to identify individuals. Yes I understand that all clinical trials and any other prospective interventional studies must be registered with an ICMJE-approved registry, such as ClinicalTrials.gov. I confirm that any such study reported in the manuscript has been registered and the trial registration ID is provided (note: if posting a prospective study registered retrospectively, please provide a statement in the trial ID field explaining why the study was not registered in advance). Yes I have followed all appropriate research reporting guidelines, such as any relevant EQUATOR Network research reporting checklist(s) and other pertinent material, if applicable. Yes The individual-level data underlying this article were subject to ethical approval and cannot be shared publicly due to data protection laws in each participating country.