@crossref
#DOAJ #OpenAccess #Crossref #metadata #LMIC
See details https://blog.doaj.org/2026/03/12/renewed-partnership-doaj-and-crossref-focus-on-equitable-scholarly-metadata-and-global-support/
In our new paper we were synthesised primary research into the experiences of adolescents concerning their #diabetes #SelfManagement after participating in a diabetes education program
https://journals.sagepub.com/doi/full/10.1177/26350106261422691
- We only found papers relating to T1DM (and only n=4)
- Experiences split into (i) general experience of self management, and (ii) barriers/facilitators in their environment
- All studies were conducted in Western/ #HIC countries
#LMIC #GlobalHealth
✔️ WHO checklist usage higher in first referral (99.4%).
📉 No significant difference in 30-day mortality between hospitals.
#GlobalSurgery #HealthcareResearch #LMIC #Pub2Post
https://tnyp.me/k32Aqpbj/m
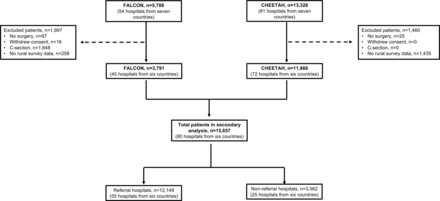
First referral hospitals, often known as district hospitals, are neglected in the discourse on universal health coverage in low-income and middle-income countries (LMICs). However, these hospitals are important for delivering safe surgery for 313 million people. This study aims to understand the structures, processes and outcomes of patients undergoing surgery in these centres in LMICs. This is a preplanned secondary analysis using data from two high-quality randomised controlled trials undergoing major abdominal surgery across six LMICs. Type of hospital was the main explanatory variable, defined according to the WHO taxonomy as first referral (ie, district or rural) and referral (ie, secondary or tertiary). Of the included 15 657 patients across 80 hospitals from 6 countries, 3562 patients underwent surgery in first referral and 12 149 patients underwent surgery in referral centres. First referral centres have lower full-time surgeons (median: 1 vs 20, p<0.001) and medically trained anaesthetists (28.6% vs 87.1%, p<0.001) compared with referral centres. Patients undergoing surgery in first referral centres were more likely to have lower rates of American Society of Anaesthesiologist (ASA) grades III–V (8.1% vs 22.7%, p<0.001), but higher rates of emergency procedures (65.1% vs 56.6%, p<0.001). In first referral centres, there was a significantly higher use of WHO surgical safety checklist (99.4% vs 93.3%, p<0.001) compared with referral centres. In adjusted analyses, there were no differences in 30-day mortality (OR 1.09, 95% CI 0.73 to 1.62) and surgical site infection (OR 1.30, 95% CI 0.89 to 1.90) between first referral and referral centres. Postoperative mortality and surgical site infection remain similar between first referral and referral centres in LMICs. There may be a clear need to upscale surgical volume safely in first referral centres to meet global surgical needs. High-quality research is needed to drive safe expansion of surgical workforce and strengthen referral pathways within these surgical health systems in LMICs.
seriesBMF test : Comparison of surgical care between first referral and referral hospitals in LMICs:
#GlobalSurgery #HealthCare #LMIC #NIHR #FALCON #ChEETAh #Pub2Post tnyp.me/k32Aqpbj
Instead of halting exports of life-threatening pesticides banned within the bloc, the European Union has continued — and even increased — shipments to the Global South, despite its pledge to end the practice, Human Rights Watch says.
📣 Listen to Professor Andy Tatem to find out how WorldPop is changing lives and improving decision making in low- and middle-income countries in #TheWeSociety podcast from @acadsocsciences.bsky.social & #WillHutton
🔗https://www.worldpop.org/blog/the-we-society-population-data-destiny
Interesting #PhDthesis investigating the inclusion of #LMIC stakeholders in core outcome set development, pointing to continued lack of involvement, strategies, and missed opportunities to enhance COS utility
https://livrepository.liverpool.ac.uk/3186985/
Background Standardizing outcomes and their measurement is a crucial aspect of evidence-based medicine. A core outcome set (COS) is a standardized set of outcomes that researchers should measure and report. The use of COS has the potential to reduce research waste, enhance knowledge translation, and ensure that patient-relevant outcomes are always reported. However, most COS work has been led by high-income countries (HICs), leaving a gap in low- and middle-income countries (LMICs). This thesis aims to fill this gap by exploring ways to improve the development and use of COS in LMICs, using the neonatal COS development process in Kenya as a model. Methodology: To understand current practice, I undertook a systematic review to describe the extent of inclusion of LMIC stakeholders in the development and use of COS (. I conducted two online surveys to explore views on including LMIC stakeholders in COS development and use. Survey 1 targeted COS developers from HICs, and Survey 2 targeted LMIC stakeholders. In survey 2, I presented three existing COS (Pre-eclampsia, COVID-19 and Palliative care) as case scenarios, and I asked respondents whether they would use the COS (with reasons). To explore whether an existing COS, agreed predominantly by HIC stakeholders, should be adopted or adapted for the Kenyan context, I undertook key informant interviews with clinicians working in newborn units and policymakers in Kenya to understand what outcomes are important to them. I also undertook focused group discussions with caregivers/mothers who had had their neonates admitted previously to newborn units. This collaborative approach helped me understand the key outcomes from their perspective. I finally conducted a consensus meeting with key stakeholders to generate an adapted COS for use in Kenya. Key findings From the systematic review, only one in five (75 of 380, 20%) COS included stakeholders from LMICs, with only four COS projects originating from LMICs. In survey 1, 37 (49%) responses were received from 75 COS developers, 29 of whom had published them between 2015 and 2020. In survey 2, there were 81 respondents from LMICs; 26 had experience using a COS, and nine had been involved in COS development. Across the two surveys, personal research interests were a key driver for initiation/participation in a given COS project; LMIC stakeholders were most frequently involved in determining the ‘what to measure’ stage of COS development as opposed to the other COS development stages like scoping and how to measure. Respondents suggested that the sensitization of stakeholders on the usefulness of COS in LMICs, translation of Delphi and COS materials into local languages, and enhancement of feasibility of outcome measurements would help get more LMIC participants to be part of COS development. The key informant interviews and Focused Group Discussions (FGD) yielded 16 outcomes (survival, length of stay in hospital, ability to feed or weight gain or growth, cognitive ability, visual impairment or retinopathy of prematurity (ROP), impact on caregivers and wider family, financial costs to the caregiver, pain, adverse events due to medicine, respiratory distress, quality of life, sepsis, future wellbeing, jaundice, necrotizing enterocolitis (NEC), ability to touch/palpate). These outcomes were subjected to a consensus-building workshop and a final set of 12 outcomes (survival, length of stay in hospital, ability to feed or weight gain or growth, cognitive ability, visual impairment or ROP, impact on caregivers and wider family, financial costs to the caregiver, pain, adverse events due to medicines, respiratory distress, quality of life, sepsis/infections) were agreed upon. Seven outcomes were similar to the HIC COS (survival, cognitive ability, visual impairment or ROP, adverse events due to medicines, respiratory distress, quality of life and sepsis/infections). In contrast, four outcomes (NEC, brain injury on imaging, hearing impairment, and general gross motor ability) were not included in this COS. Conclusion: Although LMIC stakeholders have been increasingly included in COS development and use over time, more work is required to test the proposed strategies for enhancing COS development and use in LMICs. This could be coupled with other methodological enhancements, such as documenting the adoption or adaptation of existing COS in an LMIC setting, which has the potential to enhance COS utility, as demonstrated in this thesis.
New information on our #CapacityBuilding workshop!
This is an excellent opportunity for experts in our joint action to gather and exchange knowledge on #WastewaterSurveillance and #EnvironmentalSurveillance tools.
We explicitly invite participants from #LMIC to join for free!
Registration open from September 6th.
Links to follow up:
The COSMOS set
https://gh.bmj.com/content/9/8/e015120.info
The COSmm set
https://pubmed.ncbi.nlm.nih.gov/29531104/
And a special plug for the paper presenting an interpretative phenomenological analysis of the lived experience of people with
#multimorbidity in low- and middle-income countries based on the interview data from this study
pubmed.ncbi.nlm.nih.gov/38262681/
Introduction The burden of multimorbidity is recognised increasingly in low- and middle-income countries (LMICs), creating a strong emphasis on the need for effective evidence-based interventions. Core outcome sets (COS) appropriate for the study of multimorbidity in LMICs do not presently exist. These are required to standardise reporting and contribute to a consistent and cohesive evidence-base to inform policy and practice. We describe the development of two COS for intervention trials aimed at preventing and treating multimorbidity in adults in LMICs. Methods To generate a comprehensive list of relevant prevention and treatment outcomes, we conducted a systematic review and qualitative interviews with people with multimorbidity and their caregivers living in LMICs. We then used a modified two-round Delphi process to identify outcomes most important to four stakeholder groups (people with multimorbidity/caregivers, multimorbidity researchers, healthcare professionals and policymakers) with representation from 33 countries. Consensus meetings were used to reach agreement on the two final COS. Registration: <https://www.comet-initiative.org/Studies/Details/1580>. Results The systematic review and qualitative interviews identified 24 outcomes for prevention and 49 for treatment of multimorbidity. An additional 12 prevention and 6 treatment outcomes were added from Delphi round 1. Delphi round 2 surveys were completed by 95 of 132 round 1 participants (72.0%) for prevention and 95 of 133 (71.4%) participants for treatment outcomes. Consensus meetings agreed four outcomes for the prevention COS: (1) adverse events, (2) development of new comorbidity, (3) health risk behaviour and (4) quality of life; and four for the treatment COS: (1) adherence to treatment, (2) adverse events, (3) out-of-pocket expenditure and (4) quality of life. Conclusion Following established guidelines, we developed two COS for trials of interventions for multimorbidity prevention and treatment, specific to adults in LMIC contexts. We recommend their inclusion in future trials to meaningfully advance the field of multimorbidity research in LMICs. PROSPERO registration number CRD42020197293. All data relevant to the study are included in the article or uploaded as supplementary information.