Swansea experts awarded £1.2 million for test that could transform stroke care
The three‑year project, led by Swansea University Medical School in partnership with Swansea Bay University Health Board and the Massachusetts Institute of Technology (MIT), aims to create the first accurate test to measure how blood clots break down.
Tackling a leading cause of death
Stroke remains the fourth leading cause of death in Wales. Current treatment involves administering powerful clot‑busting drugs, but doctors have no precise way of knowing the right dose for each patient.
Professor Karl Hawkins, who is leading the project, explained:
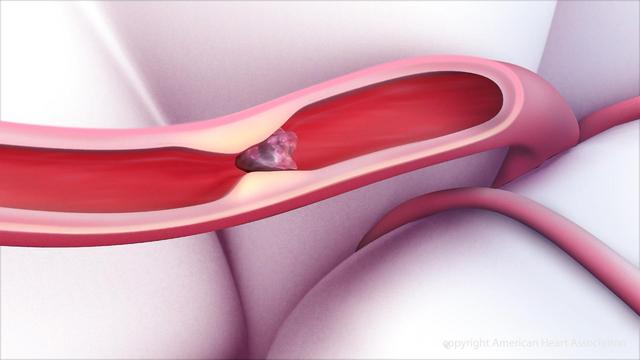
“A blood clot will form to stop bleeding, and eventually the body dissolves it. That process is called fibrinolysis. At the moment there is no accurate technique to quantify this process. Our approach, using rheology, allows us to pinpoint the exact moment a clot breaks down.”
Safer, more personalised treatment
The team hopes the test will act as a biomarker, helping clinicians predict how well clot‑busting drugs will work for individual patients. That could reduce the risk of dangerous side‑effects such as bleeding, while ensuring patients receive the most effective treatment.
Dr Suresh Pillai, Director of the Welsh Centre for Emergency Medicine Research at Morriston Hospital, said:
“These drugs cost around £600 a time and must be given within four and a half hours of symptoms. But every patient is different. We don’t know if we are over‑dosing or under‑dosing. If this test works, it would be groundbreaking. It would have a huge impact on how we manage patients.”
International collaboration
The project will draw on expertise from Swansea University’s Complex Fluids Research Group and MIT’s Professor Gareth McKinley. Initial work will test blood samples from healthy volunteers before moving to stroke patients at Morriston Hospital.
The aim is to develop a single test that can measure both clot formation and breakdown, paving the way for pharmaceutical companies to design safer, more effective medicines.
Looking to the future
Dr Pillai added that in the longer term, the test could even allow clot‑busting drugs to be given in the community rather than waiting for hospital admission.
“Every second matters in stroke care. If we can bring treatment closer to patients, the benefits for survival and recovery could be enormous.”
The £1.2 million funding has been awarded by the UKRI Engineering and Physical Sciences Research Council (EPSRC).
Related articles
- Health Board confirms temporary transfer of Gorseinon Hospital inpatient beds to Singleton
Decision taken after patient safety concerns, with assurances the hospital itself will remain open.
- A third of stroke survivors say peer support was key to recovery
Survey highlights the vital role of talking to others affected by stroke in rebuilding lives.
- Llanelli’s Minor Injuries Unit to become 12‑hour urgent care centre
Hywel Dda confirms no return to 24‑hour service as part of reshaping urgent care provision.
- Hywel Dda to explore more than 100 new ideas for local health services
Health board launches wide‑ranging review to shape the future of care across west Wales.
#bloodClot #MassachusettsInstituteOfTechnology #MIT #MorristonHospital #Stroke #StrokeResearch #Swansea #SwanseaBayUniversityHealthBoard #SwanseaMedicalSchool #SwanseaUniversity #WelshCentreForEmergencyMedicineResearch