Science for ME: News in Brief
16 - 22 Mar 2026
🧵 of highlighted #MECFS and #LongCovid research papers being discussed this week on the Science for ME forum.
@mecfs
https://www.s4me.info/threads/news-in-brief-march-2026.49238/post-682549
Science for ME: News in Brief
16 - 22 Mar 2026
🧵 of highlighted #MECFS and #LongCovid research papers being discussed this week on the Science for ME forum.
@mecfs
https://www.s4me.info/threads/news-in-brief-march-2026.49238/post-682549
Incidence age is bimodal for Myalgic Encephalomyelitis/Chronic Fatigue Syndrome, with higher severity burden for early onset disease — Mcgrath et al
"A key strength of our study is that it is the first to examine age at onset (rather than diagnosis) in a large dataset covering multiple countries with diverse healthcare systems."
Evidence of White Matter Neuroinflammation in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: A Diffusion-Based Neuroinflammation Imaging Study — Qiang Yu et al
"This study revealed significantly reduced NII-HR and NII-RF in ME/CFS patients compared to HCs." "NII-HR reflects hindered extracellular diffusion that may be affected by edema."
Intersectionality, healthcare and myalgic encephalomyelitis: Reflections from experience — Joanne Hunt
"Focusing on [ME/CFS] and drawing on my own experience as a multiply marginalised disabled person in the UK, I make a case for UK healthcare to be informed by intersectionality, not as empty rhetoric but as critical social praxis and much-needed epistemic intervention."
Microcirculatory impairment and increased arterial stiffness in pediatric Long COVID patients — Boever et al
"Our findings collectively reveal substantial microvascular impairments and increased arterial stiffness in pediatric Long COVID patients, particularly among those presenting with dyspnea."
https://link.springer.com/article/10.1007/s00431-026-06825-6
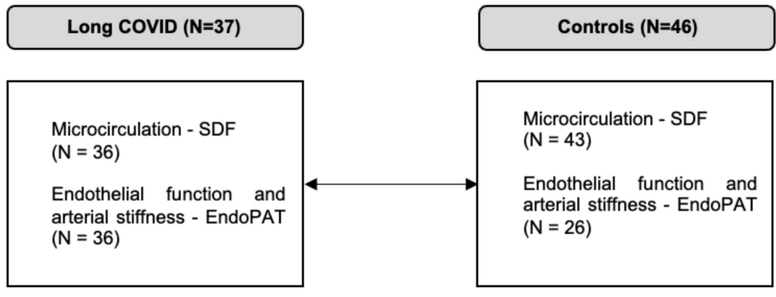
Purpose The exact pathogenesis of Long COVID remains unclear. Microvascular and endothelial dysfunction, established contributors to SARS-CoV-2-related conditions, appear to play a role in pediatric Long COVID. Methods At the Children’s University Hospital of LMU Munich, we conducted a comparative cohort study including pediatric Long COVID patients. Microcirculation was assessed using sublingual sidestream dark field (SDF) imaging, analyzing the microvascular flow index (MFI), the total vessel density (TVD), and the proportion of perfused vessels (PPV). Endothelial function and arterial stiffness were evaluated using peripheral arterial tonometry (EndoPAT), measuring reactive hyperemia index (RHI) and augmentation index (AIx@75). Results We analyzed 37 pediatric Long COVID patients (13.5 ± 2.6 years; 22 females) with persisting symptoms (> 4 weeks) and 46 healthy controls (12.4 ± 4.8 years; 21 females). Patients exhibited significant microcirculatory alterations, with reduced MFI (2.59 [IQR, 2.38–2.75] vs. 2.83 [IQR, 2.69–2.96]; p = .003), TVD (16.12 [IQR, 15.24–17.86] mm/mm2 vs. 19.38 [IQR, 17.58–20.57] mm/mm2; p < .001), and PPV (13.58 [IQR, 12.72–14.89]% vs. 17.67 [IQR, 16.60–19.32]%; p < .001). Microcirculatory changes varied with clinical phenotype and were most pronounced in patients presenting with dyspnea.We analyzed 37 pediatric Long COVID patients (13.5 ± 2.6 years; 22 females) with persisting symptoms (> 4 weeks) and 46 healthy controls (12.4 ± 4.8 years; 21 females). Patients exhibited significant microcirculatory alterations, with reduced MFI (2.59 [IQR, 2.38–2.75] vs. 2.83 [IQR, 2.69–2.96]; p = .003), TVD (16.12 [IQR, 15.24–17.86] mm/mm2 vs. 19.38 [IQR, 17.58–20.57] mm/mm2; p < .001), and PPV (13.58 [IQR, 12.72–14.89]% vs. 17.67 [IQR, 16.60–19.32]%; p < .001). Microcirculatory changes varied with clinical phenotype and were most pronounced in patients presenting with dyspnea. Conclusion: We demonstrate measurable vascular alterations in pediatric Long COVID, including microvessel reduction and increased arterial stiffness. Our findings support a role of vascular changes in Long COVID and highlight the importance of integrating cardiovascular monitoring and follow-up into the management of affected children. What is Known: • Microvascular and endothelial dysfunction appear to play a role in SARS-CoV-2-related diseases. • Adults with Long COVID show persistent capillary rarefaction and endothelial impairment supporting a vascular mechanism underlying ongoing symptoms. What is New: • Pediatric Long COVID is likewise associated with significant microvascular damage and furthermore with increased arterial stiffness. • Children with dyspnea exhibit a distinct vascular phenotype characterized by marked capillary loss, indicating a potential microvascular origin of persistent respiratory symptoms.
Persistent T cell phenotypic alterations and early innate immune dysregulation as potential biomarkers of Long COVID — Marina Perez-Mazzali et al
Hospitalised patients. "during the acute stage of the disease, differences between patients who subsequently developed LC are mainly found in the innate immunity compartment, while 3 months after hospital discharge these differences are related to the adaptive immune system."
https://www.journalofinfection.com/article/S0163-4453(26)00056-3/abstract