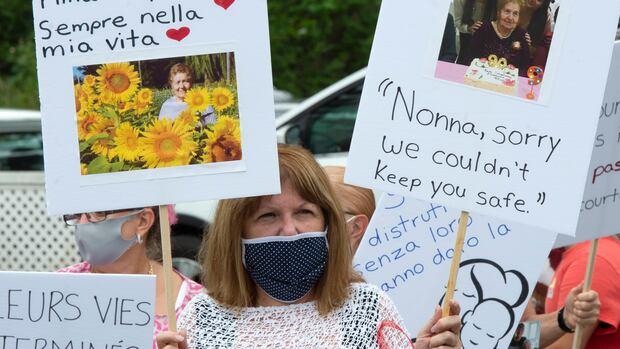SARS-CoV-2 directly infects th...
SARS-CoV-2 directly infects th...
«Studien zeigen: SARS-CoV-2 kann das #Gehör schädigen. In Mäusen dringt das Virus #ins Innenohr ein und greift Nervenzellen an. Das Spike-Protein stört wichtige Zellprozesse, was zum Zelltod führt. Hörverlust kann so auch ohne Entzündung entstehen.»
https://www.cell.com/cell-reports/fulltext/S2211-1247(26)00329-3
Sono dati parziali! A breve (però non so il giorno) inizieranno a morire tutti coloro che si sono vaccinati contro il #covid19. In meno di due secoli gli italiani hanno guadagnato 54 anni di vita. La fotografia nel nuovo report dell'Istat ‘La salute: una conquista da difendere’ https://www.quotidianosanita.it/studi-e-analisi/in-meno-di-due-secoli-gli-italiani-hanno-guadagnato-54-anni-di-vita-la-fotografia-nel-nuovo-report-dell-istat-la-salute-una-conquista-da-difendere/
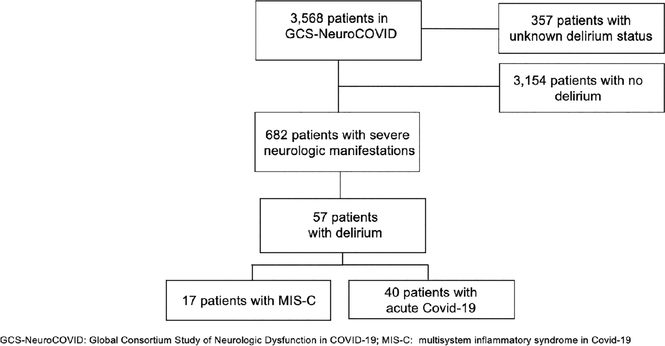
Delirium in Children Hospitalized with Acute COVID-19 or MIS-C: Secondary Analysis of the 2020–2021 Global Consortium Study of Neurologic Dysfunction in COVID-19 - Neurocritical Care
Background/Objective The aims of this study were to describe pediatric delirium and its association with inflammatory, neurodiagnostic, and clinical severity profiles in children hospitalized with acute coronavirus disease 2019 (COVID-19) infection or multisystem inflammatory syndrome in children (MIS-C). Methods We performed a secondary analysis of a multicenter, prospective observational cohort study including hospitalized children (< 18 years) with confirmed acute COVID-19 infection or MIS-C enrolled between 1 January 2020 and 31 July 2021 at 46 hospitals across ten countries participating in the Global Consortium Study of Neurologic Dysfunction in COVID-19 (GCS-NeuroCOVID). Results Among 3211 patients, 57 (1.8%) had documented delirium. Delirium was more common in MIS-C than in acute COVID-19 (3.6% vs. 1.5%, p = 0.004). Children with delirium had higher inflammatory markers (e.g., C-reactive protein, ferritin, D-dimer, procalcitonin) and more frequently presented with severe neurologic manifestations (all p < 0.001). Patients with delirium underwent more neurodiagnostic testing (p < 0.001). Among children with delirium who received electroencephalogram (EEG) testing, abnormalities were universal (n = 23). Delirium was associated with longer hospital stays (median 17 vs. 4 days; p < 0.001), higher mortality (7.5% vs. 1.1%; p = 0.01), and worse functional outcomes, including higher rates of new disability at discharge as assessed by Pediatric Cerebral Performance Category (PCPC; 22.5% vs. 1.7%, p < 0.001) and functional status scale (FSS; 22.7% vs. 2.1%, p = 0.001). Conclusions Delirium in a select group of patients with pediatric severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)-related illness was associated with systemic inflammation, severe neurologic injury, and worse clinical outcomes in a multicenter cohort. These findings underscore the importance of routine delirium screening and intervention in children hospitalized with SARS-CoV-2-related illnesses and other inflammatory conditions.
Stand with science by choosing evidence, sharing knowledge, trusting facts, and supporting policies that protect health across communities and environments.
#WorldHealthDay #PublicHealth #InfectionPrevention #COVID19 #LongCOVID
#体重 : 70.1kg
#検温
朝 : 36.4度
#パルスオキシメーター
朝 : 98%
#COVID19
症状 発熱:↑
空咳:ある
倦怠感:いつも
痰:少し
嗅覚・味覚障害:なし
息切れ:なし
筋肉・関節痛:腰が痛い
喉の痛み:なし
頭痛:なし
悪寒:なし
吐き気:なし
鼻詰まり:なし
下痢:なし
喀血:なし
結膜充血:なし
A Quebec judge has authorized a class-action lawsuit against a private long-term care home in Montréal-Nord over alleged mismanagement of a COVID-19 outbreak in 2020, during which at least 68 residents died.
https://www.cbc.ca/news/canada/montreal/quebec-covid-deaths-class-action-private-care-home-9.7155123?cmp=rss
The lawsuit is seeking damages on behalf of all the people who resided in the home between April 9 and June 26, 2020, including their spouses, caregivers, and children.
#Canada #Health #COVID19 #longtermcarehome
https://globalnews.ca/news/11767831/quebec-long-term-care-home-class-action-lawsuit-covid/
The lawsuit is seeking damages on behalf of all the people who resided in the home between April 9 and June 26, 2020, including their spouses, caregivers, and children.
#Canada #Health #COVID19 #longtermcarehome
https://globalnews.ca/news/11767831/quebec-long-term-care-home-class-action-lawsuit-covid/